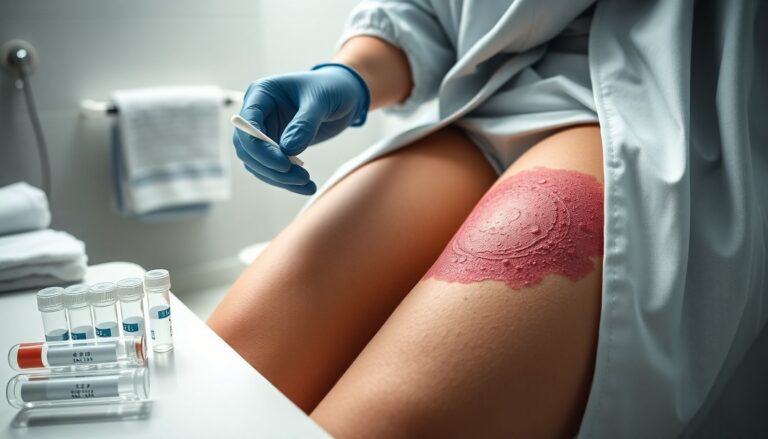
The appearance of a persistent, itchy rash can be confusing: it may look like common jock itch or athlete’s foot, yet respond poorly to over-the-counter creams. In recent months, public health clinics and community advocates have been encountering a fungal agent labeled Trichophyton mentagrophytes genotype VII — abbreviated TMVII — which behaves differently than many familiar surface fungal infections. The story of one person who noticed a scaly, painful rash after a shower on March 13 and sought care highlights how awareness often outpaces clinical systems; their local provider initially did not recognize the emerging pattern and needed to look the organism up.
TMVII is not brand new to science: the earliest documented global case dates to France in March 2026, and the first U.S. report occurred in 2026 when a traveler developed a genital lesion after visiting parts of Europe and California in June 2026. Since then, clusters including a large grouping in Minneapolis in July 2026 have prompted renewed attention. Public health observers worry about slow testing and under-recognition, especially in populations where outbreaks have concentrated, and draw lessons from past gaps in responses to infections that predominantly affected queer communities.
What TMVII is and how it looks
TMVII is a variant of a dermatophyte fungus often grouped under the broader label ringworm. Clinically it can begin with an itchy, scaly rash in the groin, buttocks, face or other sites and may progress into raised, flaking patches or painful lesions that sometimes contain pus. Unlike many tinea infections, TMVII frequently fails to clear with standard topical agents and has been shown to respond to two main systemic medications: terbinafine and itraconazole. Some clinicians add topical antifungals such as luliconazole or ketoconazole to support healing, but oral therapy is often required.
How TMVII spreads and why it can go unnoticed
Transmission routes
Transmission occurs most readily through skin-to-skin contact, which is why sexual contact has been a prominent route in the documented clusters, prompting classification as an STI in practical terms. That said, nonsexual transmission from shared towels, linens, gym equipment or close-contact sports is also possible — the fungus survives on surfaces and fabrics long enough to infect others. This mixed transmission profile means settings such as locker rooms, teams and communal living spaces are relevant to control efforts.
Testing delays and implications
The interval between exposure and symptom onset — the incubation period — tends to be a few weeks, and standard diagnostic processing for dermatophytes can take several weeks to identify TMVII specifically. Public health clinicians have cautioned that these delays create a window for onward spread before laboratory confirmation. In many areas, testing infrastructure and clinician familiarity lag behind community reports, which raises the risk the organism has circulated more widely than surveillance currently shows.
Diagnosis, treatment and practical prevention
Recognizing and responding
If you develop an itchy, migrating rash around the genitals, buttocks, face or extremities that does not improve with topical treatment, speak to a clinician about testing. The usual first-line lab technique is a fungal KOH prep, which may detect a dermatophyte, but identifying the genotype that indicates TMVII can take several additional weeks. Some public health guidance, for example protocols released by Minnesota’s health authorities, recommends initiating oral antifungal therapy right away rather than waiting for confirmation.
Treatment and harm reduction
Effective management typically involves systemic therapy with terbinafine or itraconazole, sometimes combined with topical antifungals. Treatment duration should be guided by clinical response and public health advice; experts often recommend continuing therapy for a period after visible resolution to reduce relapse risk. To reduce transmission: avoid sharing towels or bedding with someone who has an active infection, limit close contact while lesions are present, and inform sexual partners if you test positive or suspect exposure. Adding TMVII screening to routine sexual health panels may be sensible for those in higher-risk networks.
Community action and public health
Community organizations and clinicians are already filling information gaps by producing plain-language resources and outreach. Collaborations among infectious disease specialists, community clinics and national agencies aim to expand testing, standardize treatment guidance and reduce stigma. The response emphasizes harm reduction: protecting networks while preserving intimacy and connection, not shaming individuals. As with other infections that disproportionately impacted queer communities, advocates argue that timely research funding and culturally competent communication are essential to control.
Awareness, timely treatment, and modest behavioral adjustments can limit spread while scientists and health departments build better surveillance and care pathways. If you suspect you may have TMVII, consult a healthcare provider, ask about a fungal KOH test, and discuss starting oral therapy if clinical suspicion is high.